Page 7 - ESGO - Vulvar cancer - Complete report_fxd2
P. 7
5 Summary of guidelines
5.1 Diagnosis and referral
In any patient suspected for vulvar cancer, diagnosis should be established by a punch/incision biopsy.
Excision biopsy should be avoided for initial diagnosis, as this may obstruct further treatment planning.
In patients with multiple vulvar lesions, all lesions should be biopsied separately with clear
documentation of mapping.
All patients with vulvar cancer should be referred to a Gynaecological oncology centre GOC and
treated by a multidisciplinary gynaecological oncology team.
5.2 Staging system
Vulvar cancer should be staged according to FIGO and/or TNM classification1.
5.3 Preoperative investigations
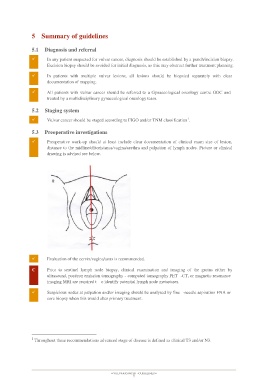
Preoperative work-up should at least include clear documentation of clinical exam size of lesion,
distance to the midline/clitoris/anus/vagina/urethra and palpation of lymph nodes. Picture or clinical
drawing is advised see below.
Evaluation of the cervix/vagina/anus is recommended.
C Prior to sentinel lymph node biopsy, clinical examination and imaging of the groins either by
ultrasound, positron emission tomography - computed tomography PET -CT, or magnetic resonance
imaging MRI are required t o identify potential lymph node metastases.
Suspicious nodes at palpation and/or imaging should be analysed by fine -needle aspiration FNA or
core biopsy when this would alter primary treatment.
1 Throughout these recommendations advanced stage of disease is defined as clinical T3 and/or N3.
VULVAR CANCER - GUIDELINES
7